In our latest edition, we spoke to Mike Hurley, creator of ESCAPE-pain – a rehabilitation programme for people with chronic joint pain. Mike is currently a Professor of Rehabilitation Sciences at St George’s University of London & Kingston University as well as Clinical Director for the Musculoskeletal theme at Health Innovation Network.
Tell us about your innovation in a sentence
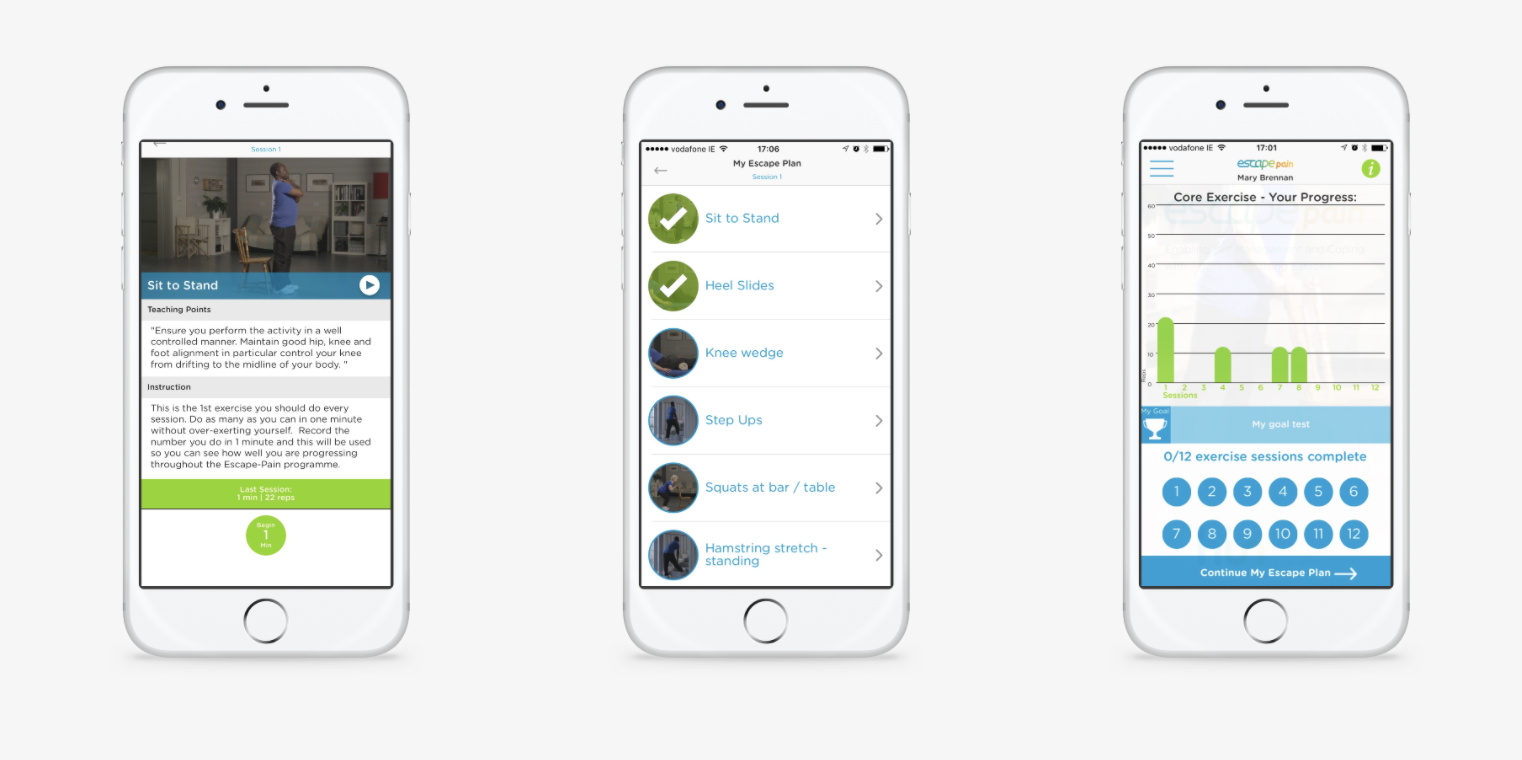
ESCAPE-pain “does exactly what is says on the tin”, it’s a rehabilitation programme for older people with chronic knee or hip pain (often called osteoarthritis) that helps participants understand why they have pain, what they can do to help themselves cope with it, and guides them through an exercise programme that helps them realise the benefits that can be attained from being more physically active.
What was the ‘lightbulb’ moment?
Not sure it was a lightbulb moment, it was more like one of the low energy lights slowly coming on! But there were two turning points that have led to ESCAPE-pain.
The first was realising the impact of pain on people’s everyday physical and psychosocial function was as important to them as the sensation of pain itself, and that addressing these impacts is as important as minimising pain.
The second was realising the importance muscle plays in causing joint pain and joint damage. We used to think joint pain was caused by damage to joints that resulted in pain, this stopped people doing their regular activities, which caused muscle weakness and makes the joint susceptible to further damage. However, we highlighted muscles are very important for protecting our joints from abnormal movement and suggested impaired muscle function that occurs as we get older may initiate joint damage. Thus, muscle is a cause rather than simply a consequence of joint damage. If that’s true then maintaining well-conditioned muscles through exercise-based rehabilitation programmes, we might prevent or reduce joint pain and damage, and improve people’s quality of life.
Coupling the first light bulb moment – addressing the psychosocial impact of pain – with the second light bulb moment – experience and understanding of the value of exercise – gives us ESCAPE-pain.
What three bits of advice would you give budding innovators?
- Prove your innovation works – if people aren’t convinced it is useful to them why would they use it?
- Surround yourself with a team of clever, hardworking people who believe in you and the innovation.
- Keep your eyes on the prize – wide implementation – and be prepared for lots of ups and downs and hard work convincing the multitude of non-believers that your innovation works.
What’s been your toughest obstacle?
Some of the conversations we had with commissioners would have been laughable if they weren’t so depressing. Financial pressures mean people delivering the programme continually want to reduce the number of sessions, but we know doing that reduces its effectiveness. And even though commissioners were often convinced about the need for the programme and wanted to do the right thing, the requirement to focus on short term benefits meant that anything taking more than a year to show benefits, whether health or cost, was of little interest. Many felt unable to invest in services where the benefits are felt by other parts of the health system, for example taking the pressure off primary care. Often commissioners could hear the madness of what they were saying even as they articulated it, but that didn’t change anything. It was tough and these issues really do slow the spread of innovation.
What’s been your innovator journey highlight?
Getting the unwavering backing of the HIN. In late 2012, I was about to give up on getting ESCAPE-pain adopted clinically, because there were no channels for innovative healthcare interventions to spread across the NHS and beyond. Then I answered an email enquiring about local MSK research in south London from its newly founded Academic Health Science Network, met with the Managing Director and frankly my professional life took a new, exciting and very fulfilling turn for the better.
Best part of your job now?
There are two:
Working with the MSK team is terrific and fun. They work so hard to make it everything work. It’s a privilege to work with such a lovely group of people.
The second great thing is the kick the whole team gets from the positive feedback we get from ESCAPE-pain participants. It never ceases to make me feel very humble and honoured to be able to help people.
If you were in charge of the NHS and care system, what’s the one thing you’d do to speed up health innovation?
I’d start “NICE Innovations”, a body that would screen potential (digital, models of care and service) innovations, pick the most promising, work with innovators and the health systems to find out what works (or not), why (not), and then actively promote and incentivise the health and social care systems to adopt or adapt effective innovations. Its kind of happening at the moment but feels fragmented, so it needs to be brought together to make it more effectual and “given teeth”.
A typical day for you would include..
The great thing about my work is that there is no typical day. I usually wake about six, make a cup of tea and listen to the news on the radio before heading into the new day. That could involve writing papers, grants, presenting at conferences, attending meetings at the HIN or St George’s, lecturing, mentoring students or clinicians, figuring out how to get our MSK work seen and adopted.
Find out more about ESCAPE-pain by visiting the website at www.escape-pain.org or following them on twitter @escape-pain