Transforming Lower Limb Wound Care Programme
To find out more about the aims, key areas of work, and our partners, visit our information hub.
The burden of chronic lower limb wound care is both a large and growing issue in England, accounting for at least 42% of all wounds in the UK. Hundreds of thousands of people in the UK live day-to-day with painful and slow-healing lower leg wounds such as leg ulcers. Due to their slow healing nature, these lower limb wounds have significant costs to the NHS every year. In 2019, the estimated associated healthcare cost of leg ulcers in England was £3.1 billion per annum (based on an estimate of 739,000 leg ulcers). Without action, prevalence is projected to rise by 4% per year to over 1 million by 2036, driven by slow healing rates and wound recurrence.
To find out more about the aims, key areas of work, and our partners, visit our information hub.
The Health Innovation Network (HIN) South London has been commissioned by the South East London (SEL) Integrated Care Board’s (ICB) System Sustainability Programme to support the transformation of lower limb wound care across the patch.
Across south east London, up to 5000 people are living with often painful and slow-healing lower leg wounds such as leg ulcers each year. The estimated prevalence of venous leg ulcers in the UK is between 0.1–0.3%, increasing with age.
Chronic lower limb wound
This describes a wound below the knee that are slow, or fail, to heal.
Leg ulcer
Venous leg ulcer
It typically occurs in the gaiter area of the leg (from the ankle to mid-calf). It occurs in the presence of venous disease and is the most common type of leg ulcer, accounting for 60–80% of cases.
The Transforming the Lower Limb Wound Care Programme addresses the challenges in lower limb wound care across all six south east London boroughs to support the transformation of lower limb wound care in line with the National Wound Care Strategy Programme (NWCSP) recommendations.
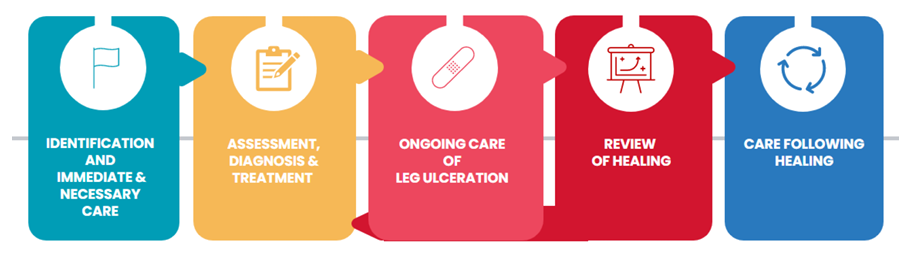
The NWCSP developed the leg ulcer best practice bundle which has the following key recommendations:
Identification and immediate and necessary care
People presenting with leg ulcers require screening for the NWCSP ‘red flag’ symptoms or conditions, the provision of immediate and necessary care (including mild graduated compression where appropriate) and onward referral for a comprehensive assessment.
Assessment, diagnosis, and treatment
Complete a comprehensive assessment within 14 days of initial presentation, diagnose and identify the causes of non-healing and develop and initiate a treatment plan designed to address those causes. For those with suspected venous leg ulceration and an adequate arterial supply, strong compression therapy should be offered.
Ongoing care of leg ulceration
At each dressing change, continue to screen for ‘red flag’ symptoms or conditions, and consider the effectiveness of the treatment plan and escalate any concerns.
Review of healing
Periodically review healing by completing an ulcer assessment, reviewing the effectiveness of the treatment plan at 4-weekly intervals, and escalating any deterioration or delays in healing in accordance with local pathways.
Care following healing
Provide appropriate care, according to the underlying cause of ulceration, to reduce the risk of recurrence.
The document provides a structured capability framework for all staff delivering wound care, covering underpinning principles, assessment, diagnosis and ongoing management.
If you are a healthcare professional based in south east London and you provide care for patients with lower limb wounds, please contact us to find out more.
Contact us