Adapting Diabetes Care to the Challenges of Covid-19
May 27, 2022As part of Type 2 Diabetes Prevention Week we hear from the HIN's Kate Rawlings on the You & Type 2 programme, and how it was adapted to the challenges of Covid-19.
Post Title
Since early 2020 organisations across the world have been asking “How do we adapt and respond to Covid-19?”, and nowhere was this more true than in our own halls at the HIN (or virtual halls, as they soon became).
Since 2018 the HIN has worked with NHS South West London Clinical Commissioning Group to develop a personalised care and support planning pathway known as “You & Type 2” for people living with type 2 diabetes. Like with other healthcare services, its delivery was significantly challenged by the emergence of Covid-19. However, with this challenge also came opportunity, and the HIN launched two new branches of You & Type 2 to support people living with diabetes in light of Covid-19: @ Home and Risk Stratification.
@ Home
As the pandemic gained momentum, more and more pressure was being placed on primary care practices, who were forced to prioritise emergency care and reduce face-to-face contact. This often meant a halting routine checks, including annual diabetes care reviews.
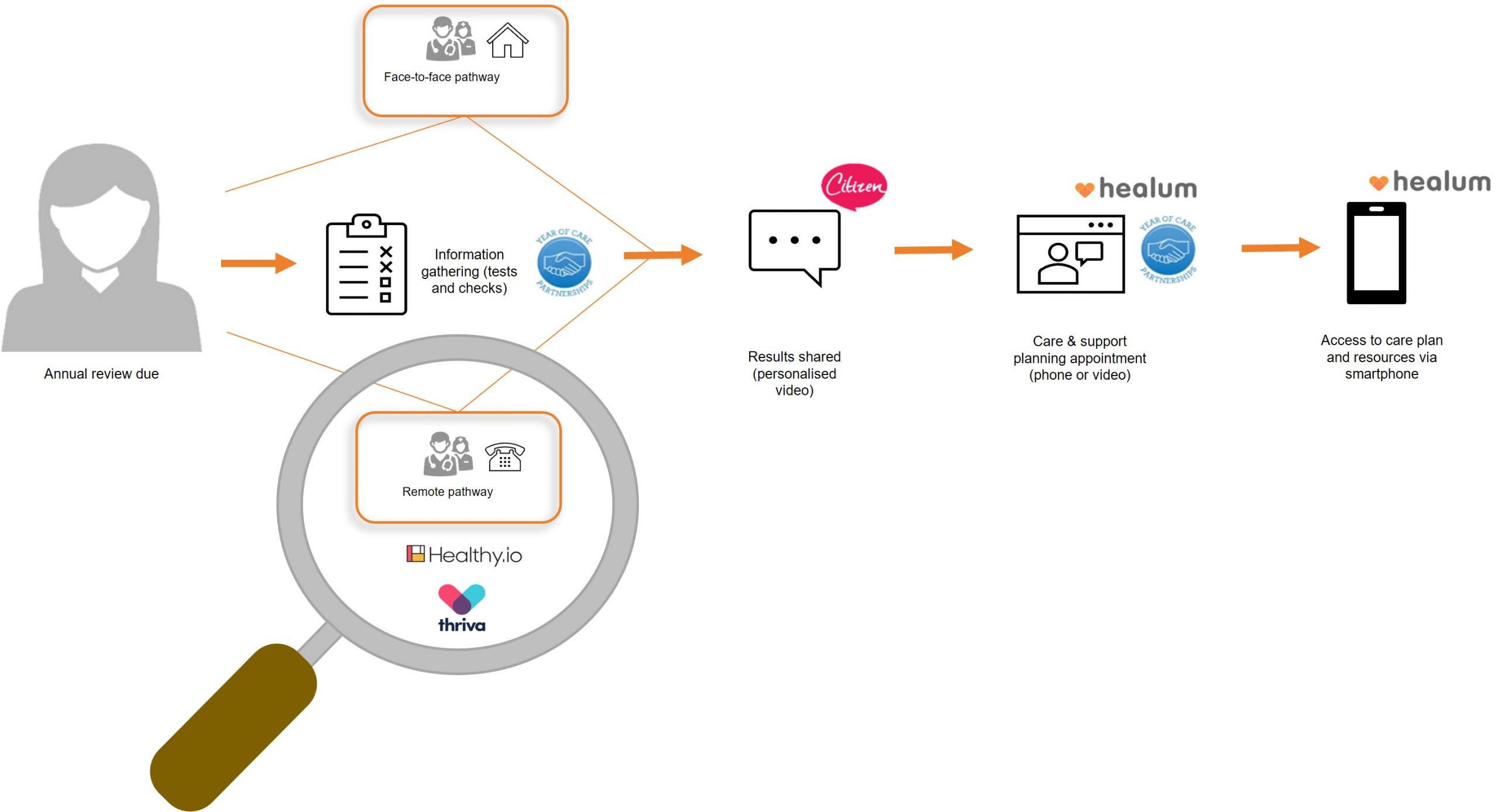
You & Type 2 was temporarily paused, however, with the help of remote technology providers Thriva and Healthy.io, a remote monitoring pathway was developed. The @ Home pathway allowed people with diabetes to receive a free home blood testing kit, urine kit and blood pressure machine in the post. Following the tests, a care planning phone call allowed for seven of the eight key care processes to be completed remotely.
Risk Stratification
Identifying and prioritising high-risk populations was an important part of the Covid-19 pandemic response. It quickly became apparent that people with diabetes were at higher risk of severe illness should they contract COVID-19, but also at risk of their diabetes worsening with the halting of routine care.
Building on existing frameworks produced by the London Clinical Networks and UCL Partners, and with the support of clinical experts, the HIN developed a risk stratification framework. This framework consolidated general and disease specific criteria to focus on people at high risk, but not currently under secondary care. It could be loaded straight into EMIS and created a list for GP practices of people with diabetes at high risk for follow up. This allowed practices to focus their limited resources appropriately.

Evaluation
Initial feedback on the pathways is positive. Over 100 people have used the @ Home pathway, and users have praised it for its convenience. Four practices across South West London have been trained to use the risk stratification tool. Full evaluations are being completed and will be released in the coming months.
Although borne out of the restrictions placed on routine care by COVID-19, these pathways show how the NHS can innovate and adapt in long term disease management to make services more convenient to their population, and how to prioritise interventions for those most in need.


