A co-designed approach to scoping and evaluating the digital health technology getUBetter
February 2, 2022Project overview
getUBetter provides digital self-management for individuals with musculoskeletal (MSK) conditions.
During 2019, the HIN led work to map the getUBetter app against the NICE evidence framework for Digital Health Technologies. Following this, an evaluation was scoped and conducted between 2019 and 2021 the HIN worked with a range of partners to explore the effectiveness of getUBetter.
We summarise the key findings including how easy people found getUBetter to use and the impact it had on the treatment for their condition.

A collaborative approach to real-world evaluation
Co-production with stakeholders has been a core principle throughout the evaluation with getUBetter. The HIN led a collaborative partnership to scope, design and deliver the digital health technology (DHT) evaluation, working with getUBetter, St George’s University Hospitals NHS Foundation Trust, the University of West of England, Wandsworth Clinical Commissioning Group (CCG) patient and public involvement (PPI) lead and Digital Health.London (DH.L). A novel aspect has been operationalising the NICE Evidence Standards Framework for DHTs so that these underpin the evaluation.
The first phase was to develop an approach that allowed us to use the standards framework to map the existing evidence-base for getUBetter against each tier. The outputs from the mapping were presented and validated at a stakeholder workshop with specialists in MSK conditions and digital evidence generation. This group then worked together to design an evaluation to ensure it addressed evidence gaps that aligned with the requirements set out in the evidence standards framework (ie behaviour change techniques and effectiveness). Colleagues at the University of the West of England undertook work to develop the evidence-base around behaviour change techniques and the HIN worked in partnership with getUBetter and provider organisations to evaluate aspects of effectiveness.
The evaluation plan
A detailed mapping exercise determined the getUBetter app met evidence standards for Tier A, B and C DHT.
These corresponded to previously named tiers 1, 2, 3a and 3b.
- Tier 1 (System Impact) evidence for effectiveness standards: met
- Tier 2 (Understanding and Communicating) evidence for effectiveness standards: met
- Tier 3a (Interventions) evidence for effectiveness standards – use of appropriate behaviour change techniques: met (best practice standard)
- Tier 3b (Interventions) evidence for effectiveness standards – demonstrating effectiveness: partially met (minimum standard)
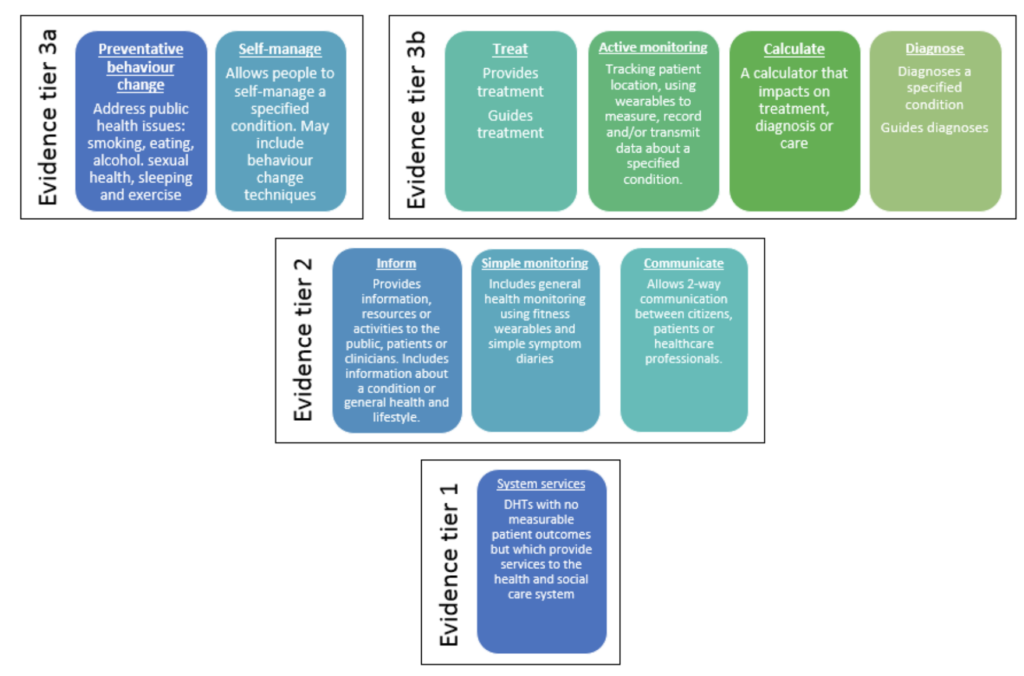
Caption: DHTs classified by function and stratified into evidence tiers (source: NICE evidence standards framework for digital health technologies [1])
A mixed-methods evaluation was co-produced involving getUBetter, Wandsworth Clinical Commissioning Group (CCG), St George’s University Hospitals NHS Foundation Trust, DH.L, the University of West of England, and the HIN.
The aim was to explore several aspects of the ‘demonstrating effectiveness’ category for condition-related outcomes, behaviour change outcomes, user satisfaction and health utilisation. Due to the ongoing Covid-19 pandemic, the evaluation was re-scoped to ensure activities could be completed within the Small Business Research Initiative (SBRI) programme funding timeline in 2021. The revised evaluation approach involved:
- An online survey sent to getUBetter users to capture respondents’ demographic profile and app usage; experiences and satisfaction; condition-related outcomes; and changes in self-management and understanding of their condition.
- An online survey of clinicians to explore awareness, use and value of getUBetter.
- Health utilisation analysis to determine resource use from primary care data comparing patients with lower back pain with non-users in a sample of 10 GP practices.
Key findings
Health utilisation
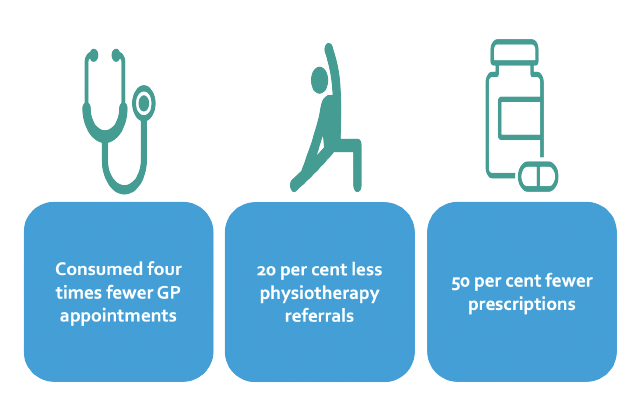
Health utilisation analysis found that 835 patients were prescribed getUBetter for lower back pain, 50 per cent of whom activated their account. Compared to non-users, getUBetter users required four times fewer GP appointments, 20 per cent fewer physiotherapy referrals and over 50 per cent fewer prescriptions.
Patient survey findings
-

80 per cent of patients had not used a health app before
80 %
-

Three quarters of patient respondents rated the app as ‘very good’, ‘good’, or ‘acceptable’.
75 %
-

55 per cent of patients reported using the getUBetter app in the past week
55 %
Most liked aspects of the app as reported by patients
- Easy to use the app
- Helps me develop skills to manage my injury/condition
- Provides relevant information according to my stage of recovery
- It gives me reassurance
It was easy to register on getUBetter (given the apps needs information to ensure I get the right advice and to keep me safe; n=151)
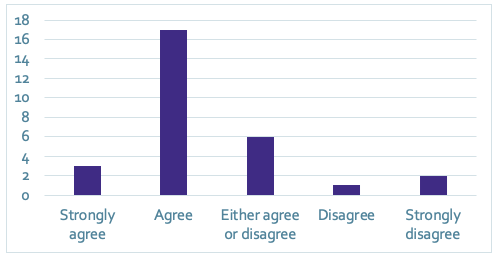
Caption: Patient respondents reported it was easy to register on the getUBetter app
‘the app is a good reminder of what a healthcare professional has said in consultation when there is little time and a lot of information to digest’
getUBetter user
Patient respondents reported that during Covid-19, the app provided a good alternative to help manage their condition. When patients were not able to get face-to-face appointments or physiotherapy, they were happy to use the getUbetter app. Patients appreciated being able to recover independently without having to see a healthcare professional.
Impact of using getUBetter (n~159)
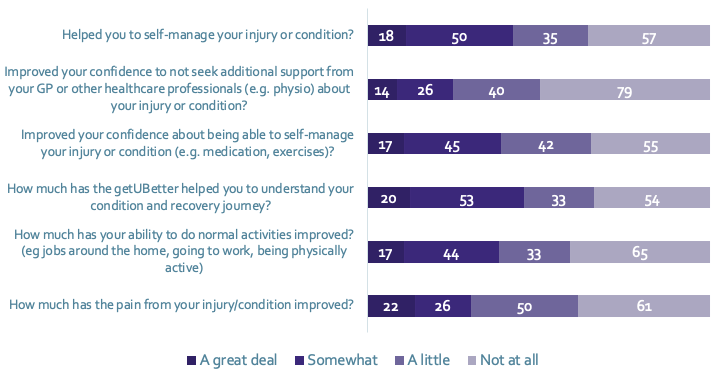
Caption: The majority of patients reported some benefit of using the getUBetter app.
Age group of respondents (n=204)
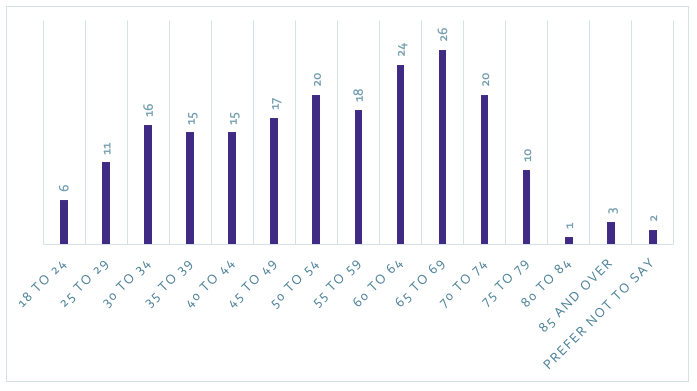
Caption: Adults across different age groups responded to the survey and reported the app easy to use
How often have you used the getUBetter app?
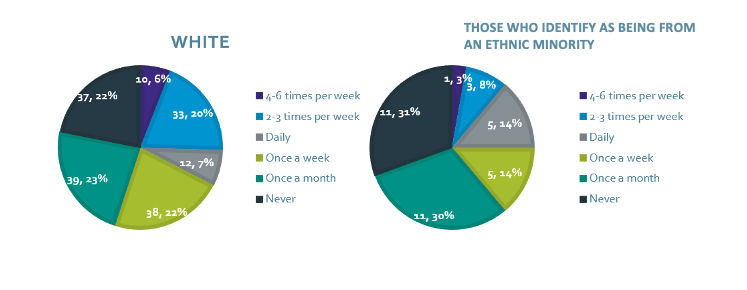
Overall rating of the getUBetter app
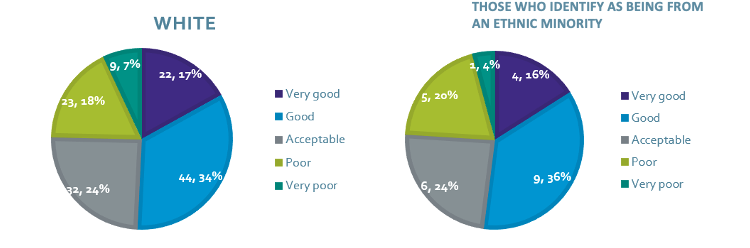
Caption: Despite most of the sample identifying as ‘white’ ethnicity, when comparing usage of the getUBetter app, there were small differences between ethnic groups. However, when comparing the overall rating of the getUBetter between ethnic groups, respondent ratings were very similar and positive across all groups.
Clinician survey findings
-

Most clinicians reported making referrals to the app
79 %
-

Most clinicians thought that the app supported patients with MSK conditions to self-manage
90 %
Outputs and contacts
An abstract was accepted for the Chartered Physiotherapy Society’s virtual conference 2021 which summarises the approach and results of the evaluation.
If you would like to learn more about the evaluation or getUBetter, please contact the team:


