A tale of my grandfathers and the revolution in cardiovascular disease prevention
Laura Semple, Programme Director for Diabetes & Stroke Prevention at Health Innovation Network, reflects on how new prevention techniques might have changed her grandparents’ lives.

I’ve often wished I’d had the chance to meet my grandfathers, Gerry and David. They were both fascinating and spirited people, who led interesting lives. Gerry travelled the world, had a successful career in industry and loved fishing for trout in the Welsh countryside. David worked in finance for London Transport and enjoyed vintage cars.
Sadly, I didn’t get to meet them because, like many people of their generation, they died too soon from cardiovascular disease in the 1970s and early 1980s.
This part of my family history is far from unique. It’s also a big reason why I find it so rewarding to be part of the movement of committed people working to prevent cardiovascular deaths in this country. February is National Heart Month and I’m thoughtful about the real progress that we’re seeing in south London in this area.
One of the main drivers of cardiovascular disease in the UK that Gerry and David grew up in was a lack of understanding around the impact of certain foods and other lifestyle aspects on heart health. It was very common to eat a high fat diet and the true scale of tobacco-related harm was not yet understood. But since the 1970s we have gained a rich understanding of the impacts of diet, exercise, tobacco and medication on heart health.
What’s more, we now have risk models, which enable us to accurately predict how likely it is that someone will have a heart attack or stroke in the next 10 years, simply by knowing their BMI, blood pressure, cholesterol and blood glucose measurements today.
This all makes me wonder just how different it could have been for Gerry and David. Not only are we now able to offer preventative care that extends lives, but crucially these are also improving the quality of those lives.
At its core, most of our work is really about giving Londoners the support they need to live full lives without the burden of diabetes and cardiovascular disease.
The first success to highlight on the prevention front is south London’s contribution to the Academic Health Science Network’s national stroke prevention programme.
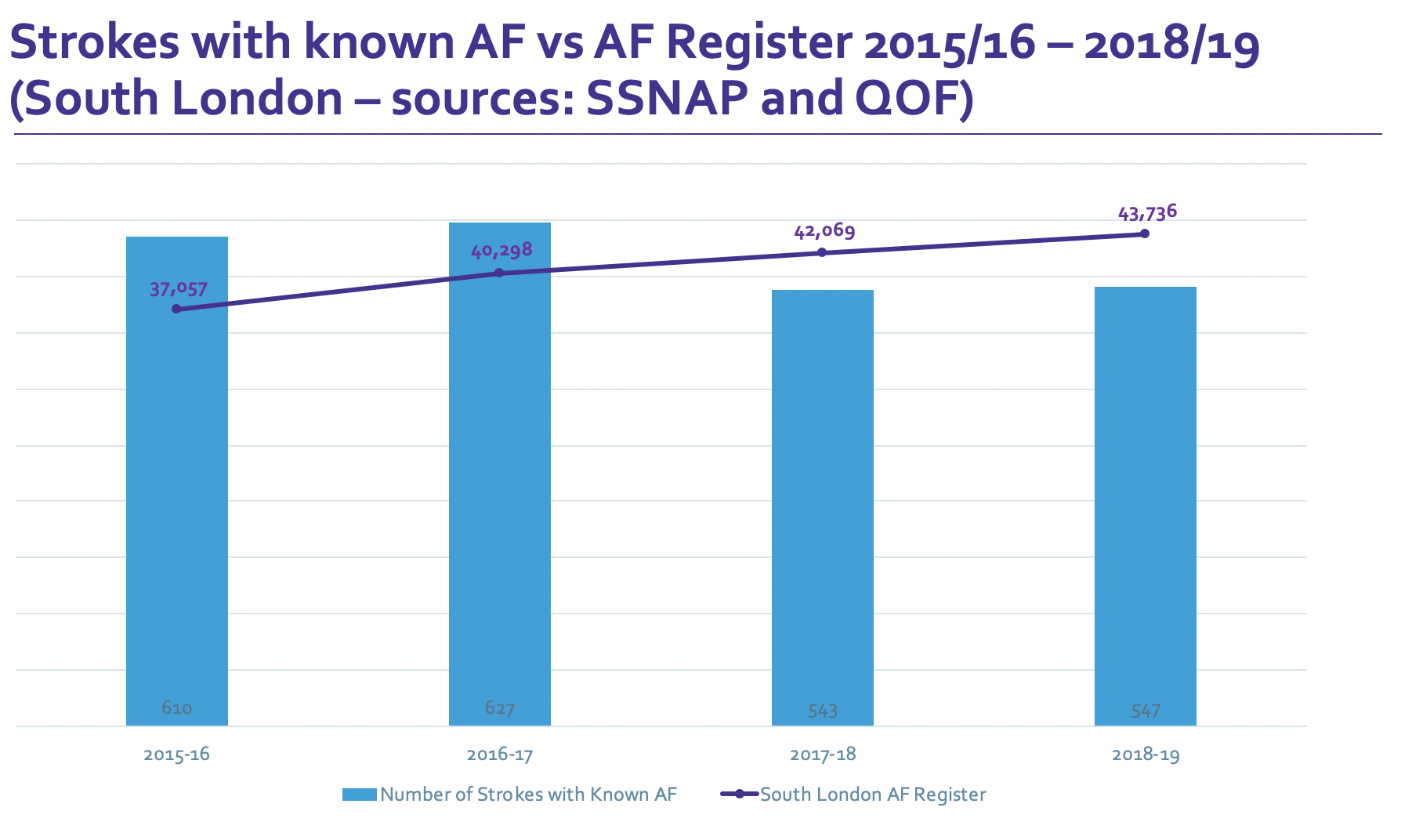
Atrial Fibrillation (AF) is one of the most common types of irregular heart rhythm and contributes to one in five strokes. If Gerry and David had been born 20 years later, there’s a good chance that they could have been two of the more than 4,500 additional south Londoners whose AF has been newly detected since 2017.
The latest national stroke audit data shows that in the two years to March 2019 there were approximately 150 fewer AF-related strokes in south London than would have been expected from the previous years’ data. This is 150 Gerrys, Davids, Simones, Ritas, Mohammeds, and many others, who are still thriving as a result. We’ve recently published the results of our innovative work in improving AF detection through mobile ECG devices here and an ongoing pilot of 14-day ECG patches on page 12 of Cardiac Rhythm News January 2020 here.
Then there’s diabetes.
This is a major driver of cardiovascular disease and it’s simply astonishing how much our experience and understanding has transformed since Gerry and David were alive. Back in the 1960s and 1970s, we were not as good at detecting type 2 diabetes, so some people lived with the condition for many years without a diagnosis, which in itself increased their risk of preventable ill health.
In general, there was far less freedom and choice for people with diabetes in how they lived their lives, with many being told to stick to rigid set diets.
But in 2020, we believe in giving people with diabetes as much freedom as possible to live the lives they want, without diabetes getting in the way. South London has a formidable partnership of colleagues committed to minimising the impact of diabetes on citizens’ lives. Together we represent 12 clinical commissioning groups, 12 local authorities, seven acute hospitals, two universities, the King’s Health Partners Institute of Diabetes, Endocrinology and Obesity, the Applied Research Collaborative, several industry partners and community organisations like the Wandsworth Community Empowerment Network The last two years has seen a major focus on type 2 diabetes prevention, with over 30,000 south Londoners referred to the NHS.
I’m curious as to what Gerry, David and their friends might have chosen if they had had access to Diabetes Book & Learn, a radical move to scrap the previous postcode lottery of self-management support for people with diabetes. In this new system, south Londoners are learning how to live well with diabetes at a time and place that works for them in their busy lives, with different languages, digital options, evening and weekend courses and telephone coaching all available.
Would Gerry and David’s employers have supported their access to diabetes education through the learnings of our Think Diabetes report?
People with type 2 diabetes are also increasingly taking charge and setting the agenda for their doctors and nurses in the innovative You & Type 2 programme in primary care.
Would Gerry and David’s employers have supported their access to diabetes education through the learnings of our Think Diabetes report? This was supported by former Labour Party deputy leader Tom Watson. Many forward-thinking employers are using the recommendations in this report to offer support directly in the workplace.
At its core, most of our work is really about giving Londoners the support they need to live full lives without the burden of diabetes and cardiovascular disease. Healthy living is far from easy. People need holistic and non-judgemental support and this is why the offer of psychological support is built into Diabetes Book & Learn and many other new services.
There is a great deal more to do to prevent cardiovascular disease and exciting plans are afoot to do even more to tackle the longstanding health inequalities in our region. For now, I’m asking everyone who has played a role in the great progress so far to take a moment this heart month to remember the strides we have made together and renew our energy to take this to the next level.
If you are keen to join the fantastic team of people saving lives by preventing cardiovascular disease in south London please visit our webpages on diabetes and cardiovascular. Alternatively, get in touch with me on laurasemple@nhs.net. This year we will be focussing on cholesterol and blood pressure as well as continuing to support our members with AF detection and improvements in diabetes care. The more collaborators we have, the more lives we can save.
I know that Gerry and David would be only too happy to see that things are different and getting even better, for the generations who came after them.
Share this Post
NB: Gerry and David are not the grandfathers’ real names.
